Atrial fibrillation (AF) is the most frequently encountered arrhythmia in clinical practice.1,2 The prevalence of AF in the United States ranges from 2.7 to 6.1 million, with 5.6 to 12 million additional cases projected by 2050.1 Medicare spending for new AF diagnoses has reached $15.7 billion per year as extrapolated from a 2004–2006 dataset, primarily driven by its complications (e.g. stroke, heart failure, tachycardia and myocardial infarction).3,4
Management of AF generally consists of preventing stroke and managing the rhythm, either by controlling the ventricular rate independent of rhythm (rate control) or by restoring and maintaining sinus rhythm (rhythm control). Maintenance of sinus rhythm is usually reserved for patients with symptoms attributable to AF, but may also be beneficial in heart failure or structural heart disease.5 Over the last 15 years, pulmonary vein or antral isolation by catheter ablation has matured as a therapeutic option for rhythm control and has been shown to have greater efficacy than antiarrhythmic drug (AAD) therapy alone.6–8 Investigation into its cost-effectiveness, however, has been limited.
Multiple studies have demonstrated that anticoagulation with warfarin or with target-specific anticoagulants is cost-effective in moderateto high-risk patients with AF.9,10 The data are more variable for catheter ablation, in part due to the heterogeneity of treatment, patient selection, and the challenge of comparing a procedure with upfront risks and costs to a daily pharmaceutical therapy with a more consistent risk and cost profile. In this review, we present key considerations in estimating the costs and effectiveness of ablation, highlighting limitations of the current literature and areas requiring additional research.
A Primer on Cost-Effectiveness Analysis
Cost-effectiveness analysis (CEA) attempts to determine the value of an intervention by comparing the costs and outcomes (clinical effectiveness) of two or more therapies.11 Value in healthcare is conceptually defined as Value = Effectiveness/Cost.
Effectiveness can be measured in the years of life gained from a therapy. However, since not all health states are equally desirable, quality-adjusted life years (QALYs) are incorporated by multiplying a “utility” value to the life-years of survival gained (where a utility of 1.0 represents ideal health). Note that this framework does not give preference to longevity or utility: 10 years of perfect health is considered equivalent to five years of health at 50 % utility. Considerations in the effectiveness of a study intervention include magnitude of effect (number of life-years or improvement in quality of life [QOL] added by procedure), efficacy (the success rate of the procedure), and complications.
Healthcare costs are usually generated from published fee schedules of reimbursements from payers, or from empirical assessments of actual reimbursements of claims (e.g. Medicare data in the US). The costs of procedures, medications and services often vary across hospitals and regions even for the same payer. Costs not only reflect out-of-pocket expenditures of the procedure or medication, but also incorporate long-term healthcare expenses, which may include complications, repeat procedures and other spending (e.g. hospitalisation fees). Costs must also be adjusted for inflation to reflect current prices.
Value is quantified with the incremental cost-effectiveness ratio (ICER) and represents a cost per QALY gained expressed as ICER = [Cost (A) – Cost (B)] / [Benefit (A) – Benefit (B)]. Larger ICERs indicate poorer cost-effectiveness. In the US, ICERs are not officially used for policy determination, but are considered by European governments such as the UK and the Netherlands. In practice, the willingness-topay threshold based on acceptability of value is $50,000USD/QALY in the US and £20,000/QALY in the UK.12 ICERs below this range are generally regarded as cost-effective. ICERs above $100,000USD/ QALY or £40,000/QALY are considered too expensive. In the case that a treatment is both less expensive and more effective than its comparator, we say that it “dominates” the alternative.
The balance between cost and effectiveness also depends on the time horizon, or duration over which the treatment’s costs and benefits are considered. Short time horizons (e.g. two to five years) can fail to capture long-term value of a therapy, particularly when there is high early cost or risk such as with a procedure. On the other hand, econometric models utilising significant assumptions over long time horizons (e.g. a lifetime) can have magnified distortion from inaccurate inputs. Investigators may also overestimate the long-term benefits of certain interventions.11,13
CEA incorporates cost and effectiveness data in several approaches. One is trial-based, where costs and benefits are calculated alongside an ongoing randomised clinical trial (RCT). The advantage of this method is that “real numbers” are gathered during the course of the comparison of interventions. Furthermore, because incremental differences in cost and QALY are of interest, randomisation helps to balance all other confounders in both groups. The disadvantage of a trial-based approach is that characteristics of randomised trial populations are often not generalisable to patients considered for the treatment in a healthcare system.14,15 Trial patients may have higher compliance, greater symptom burden, and may receive more regular or protocolled follow-up. Also, since clinical trials are costly, their time horizons are often short.
An alternative approach is a model-based study, which instead uses a set of inputs of cost, QOL and estimates of risks and benefits of treatment. Models are desirable as they can extrapolate findings over long time horizons. An example is the Markov decision analysis model, in which hypothetical patients enter various health states over the length of a set time horizon, simulating a disease course. The multiple branch points allow for the input of various clinical parameters, enabling researchers to approximate society-level populations. Unfortunately, this approach is limited by the strength of model design or inputs, which may not reflect the full heterogeneity of clinical practice and often must assume values where data do not exist. Models can be tested for their sensitivity to these input assumptions through one-way sensitivity analysis, where an assumed variable is changed over a range of values to determine its impact on the model’s outcome.
Hybrid approaches, combining trial-based utilities and cost for shortterm inputs and model-derived values for longer term inputs, have been increasingly used.16 All AF CEAs have been model-based, as existing RCTs have not reported long-term cost or QOL data.
Cost of Catheter Ablation
Costs of AF ablation range considerably between countries and even within the same healthcare system. For example, two studies in 2003 reported average procedural costs of €4,715 in France and $17,173 in the US, based on hospital billing records.17,18 A Japanese report estimated a cost range of ¥1,063,200–¥4,059,280 (2010).19 Data from government fee schedules were used to generate expenses of $21,294CAD in Canada (2007) and $26,584USD in the US 2008).20,21
Unfortunately, many of these published cost estimates incorporated into CEA analyses are over 10 years old and simply adjusting for inflation may fail to reflect present-day costs. Recently, we analysed 26,000 patients with commercial healthcare insurance in the US who underwent AF ablation between 2006 and 2011. The median cost was substantial and with considerable variation ($21,300USD; Interquartile Range 25–75 %: $12,000–$38,500USD). We also found that cost increased by 22 % from 2006 to 2011, which far exceeds the rate of healthcare inflation in the US (data unpublished).
Effectiveness and Safety of Catheter Ablation
A meta-analysis comparing AF ablation with AAD therapy included 63 studies with nine RCTs.6 The authors concluded that the single and multiple procedure success rates for maintaining normal sinus rhythm (NSR) were 57 % and 77 %, respectively (compared with 52 % on AAD alone). Of note, the mean follow-up period of their component studies was 14 months, with significant variation between studies (two to 30 months). Other trials and reviews have reported efficacy values as optimistic as 88 %.7,22–25 More recently, our group updated the Calkins review by extending its cohort through January 2012. We found the pooled success rates for single and multiple procedures to be 61±18 % and 73±14 %, respectively.8
A major limitation of these results is the considerable variation in the definition of treatment failure and method of ascertainment. Moreover, no studies evaluated QOL as a primary outcome, making assessment of utility difficult. However, other observational studies have shown that AF is associated with reductions in QOL, which improves after restoration of NSR from ablation.7,18,21,26 A utility value calculated for a 2009 CEA was 0.725 for patients having AF, with a 0.065 post-procedure improvement if patients remained in NSR.21
AF ablation also carries procedural risk, such as haemorrhage and stroke.6,27 Data from the California State Inpatient Database indicated an in-hospital complication rate of 5.1 % after ablation.27 52.1 % of the reported adverse events were vascular (44.1 % haemorrhagic). Cardiac perforation or tamponade accounted for 44 % of the complications. Less common complications included stroke (4.7 %), pneumothorax or haemothorax (1.9 %), and transient ischaemic attack (1.4 %). Only one inpatient death was reported for the cohort of 4,156. The 30-day readmission rate was 9.4 %, mostly attributable to AF recurrence. These adverse event rates are comparable to those reported in clinical trials and international site surveys.6,7,28,29 Two of these studies demonstrated higher 30-day and longer term rates of major complication with AAD treatment.6,7 In the international survey of AF ablation, the complication rate (up to 19 months out) among 181 centres who responded to the survey was 5.9 %.28 A follow-up survey published five years later found a similar major complication rate of 4.5 %.29
Cost-Effectiveness of Catheter Ablation
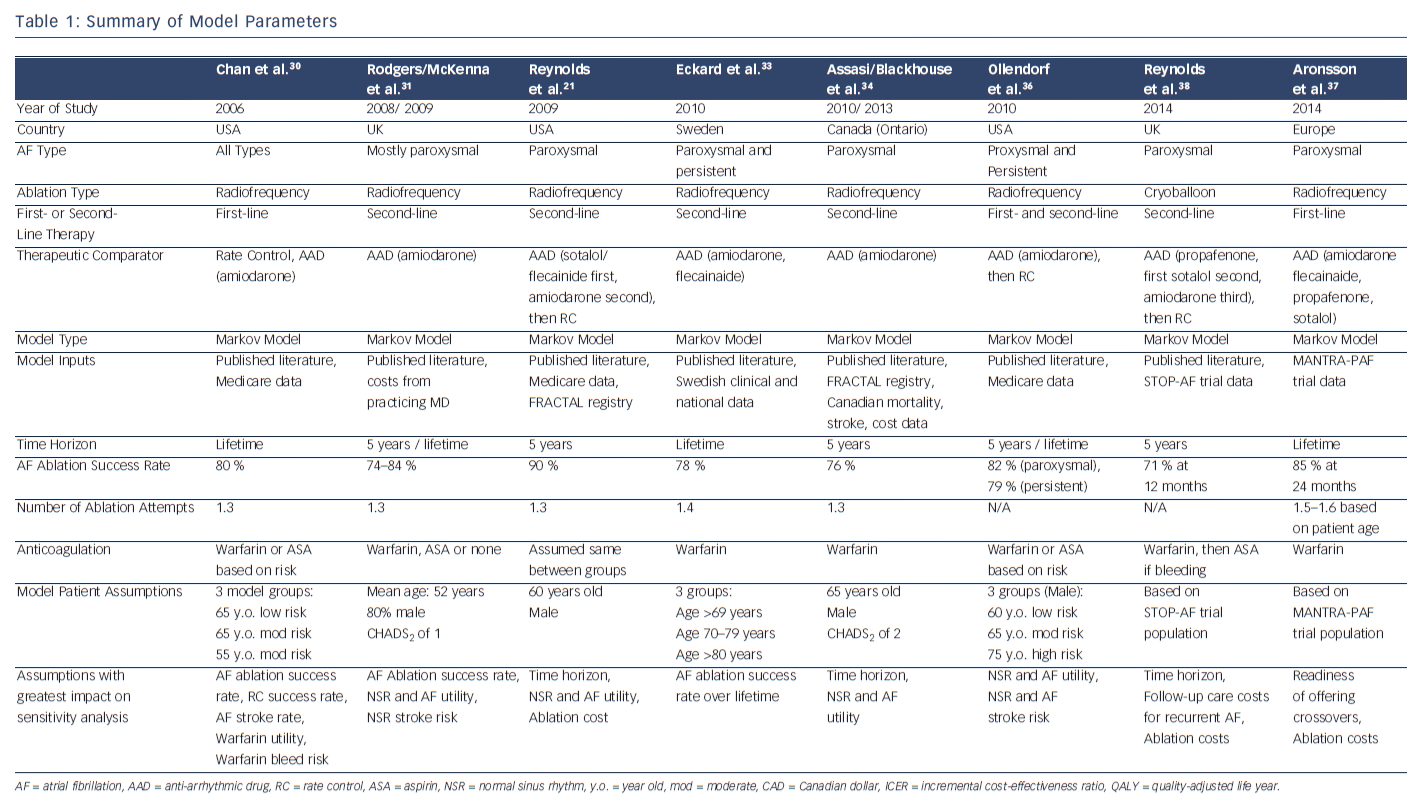
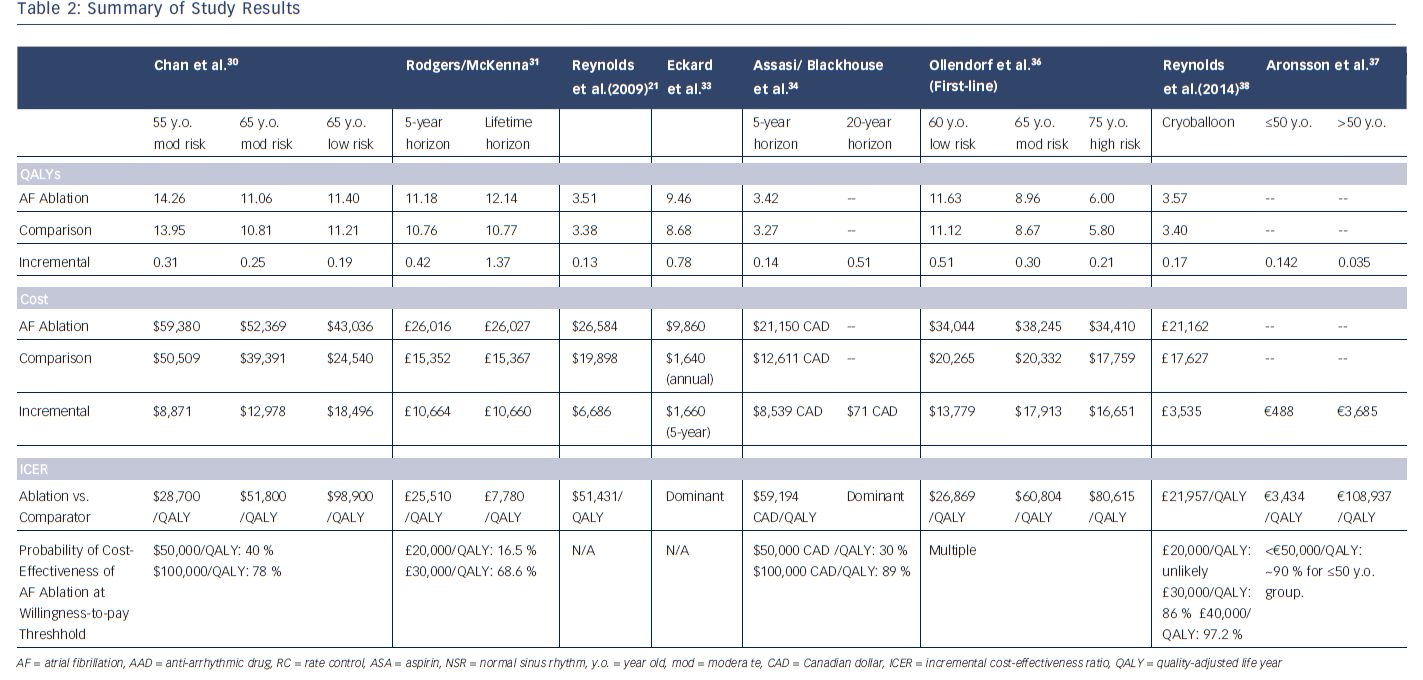
We identified eight major studies evaluating the cost-effectiveness of catheter-directed ablation of AF by performing a literature search of MEDLINE, PubMed and Web of Science for articles published between January 2006 and October 2014.21,30–38 Seven of the studies examined RF ablation, while one examined cryoballoon ablation. All the studies utilised a Markov model and reported their findings as ICERs. A compilation of the model parameters is provided in Table 1 and QALYs, costs and ICERs are summarised in Table 2. The analyses differed in type of AF considered (paroxysmal, persistent or both), the role of ablation as a first-line or second-line treatment, control group (AAD or rate control), anticoagulation regimen and time horizon. Further details of each study will be reviewed case by case below.
Chan (2006)
The first published CEA compared AF ablation to rate and rhythm control (with amiodarone) using a US societal perspective.30 Costeffectiveness over a lifetime time horizon was assessed in several patient scenarios. AF ablation vs. rate control had ICERs of $51,800USD/ QALY and $28,700USD/QALY in hypothetical patients aged 65 and 55 years, respectively, at moderate stroke risk. If the 65-year-old’s stroke risk profile was changed to low-risk, then the ICER increased to $98,900USD/QALY. Noteworthy assumptions of this model driving ICER included the cost of AF ablation, efficacy of rate control, success rate of AF ablation, utility of warfarin therapy, rate of haemorrhage on warfarin, and stroke rate of AF. The model assumed utility benefit to be near zero between NSR and AF.
Rodgers/McKenna (2008)
Subsequent CEAs analysed real-world data from the UK.31,32,39 Unlike the previous analysis, the comparator to catheter ablation was AAD, and ablation was treated as second-line therapy for patients failing AAD. For a predominantly male (80 %), younger (mean age 52 years) patient population with CHADS2 score of 1, the study yielded an ICER of £25,510/QALY over a five-year time horizon and an ICER of £7,780/ QALY over a lifetime horizon. Important assumptions of this analysis with impact on ICER included the success rate of ablation, stroke risk of NSR, and improvement in QOL in NSR compared with AF.
Reynolds (2009)
The next published study revisited the US viewpoint, evaluating ablation as second-line treatment in a 60-year-old male cohort with paroxysmal AF.21 Over a five-year time horizon, an ICER of $51,431USD/ QALY for ablation vs. AAD was obtained. The model assumed a first procedure ablation success rate of 60 % and that AAD medications would not be continued once NSR was achieved in the ablation group, as well as no difference in stroke or mortality risk between NSR and AF. Improved utility values in the NSR population compared with AF were calculated using the SF-12 and SF-36 questionnaires.40,41 Key assumptions with greatest effect on sensitivity analysis were NSR and AF utility and ablation cost.
Eckard (2010)
A CEA of the Swedish population analysing ablation versus AAD as second-line therapy over a lifetime horizon found that AAD was dominated by ablation.33 The assumption with the greatest impact on the model was the rate of NSR maintenance over a lifetime in the ablation group. As such, ICERs were calculated for annual probability of reversion to AF following ablation at 5 %, 10 %, and 15 %, yielding $8,280USD/ QALY, $26,460USD/QALY and $48,310USD/QALY, respectively.
Assasi/Blackhouse (2010/2013)
An analysis of the Canadian population determined an ICER of $59,194CAD/QALY for RF ablation compared with AAD (amiodarone) over a five-year time horizon for a base case cohort of 65-year-old male patients with paroxysmal AF and CHADS2 score of 2.34,35 Though a lifetime time horizon was not explored, the model extrapolated results over a 20-year horizon, finding ablation to be dominant over AAD. The authors noted that, contrary to the Reynolds study, their model produced a higher ICER ($86,129CAD/QALY) when assuming that restoring NSR had no impact on stroke risk. Their model was highly sensitive to AF and NSR utility, with ICERs ranging from $38,390CAD/QALY to $221,839CAD/QALY for AF disutility values of 0.08 and 0.0, respectively. Interestingly, the probability of AF recurrence following ablation was not an assumption that impacted their ICER estimate significantly.
Ollendorf (2010)
A White Paper by the Institute for Clinical and Economic Review investigated the cost-effectiveness of AF rhythm control strategies in multiple contexts.36 The project considered a variety of therapies including rhythm and rate control, catheter ablation and surgery. The group’s model utilised three hypothetical patient cohorts: a 60-year-old male group with paroxysmal AF and CHADS2 score of 0, a 65-year-old male group with persistent AF and CHADS2 of 1, and a 75-year-old male group with persistent AF and CHADS2 of 3. AF ablation was examined as both first- and second-line treatment compared with rate control as second-line treatment following failure of AAD (amiodarone). For first-line ablation compared with secondline rate control, the 60-year-old low risk group yielded an ICER of $26,869USD/QALY, the 65-year-old moderate risk group: $60,804USD/ QALY, and the 75-year-old high-risk group: $80,615USD/QALY. For second-line ablation compared to second-line rate control, the 60-year-old low risk group yielded an ICER of $37,808USD/QALY, the 65-year-old moderate risk group: $73,947USD/QALY, and the 75-year old high-risk group: $96,846USD/QALY. The authors also compared second-line catheter ablation with thorascopic off-pump surgical ablation and determined that in all three groups, catheter ablation dominated surgical ablation. Assumptions with greatest impact on one-way sensitivity were AF and NSR utility and stroke risk following AF conversion to NSR. The decreased use of warfarin following conversion to NSR, as well as the impact of warfarin on QOL, did not significantly alter the Ollendorf model.
Aronsson (2014)
A recent CEA based on the European MANTRA-PAF (Medical Antiarrhythmic Treatment or Radiofrequency Ablation in Paroxysmal Atrial Fibrillation) multicentre clinical trial determined an ICER of €50,570/QALY when comparing RF ablation with AADs as first-line therapy for a lifetime time horizon in Denmark, Finland, Germany and Sweden.37 Subgroup analysis suggested that ablation was more cost-effective in younger patients, as an ICER of €3,434/QALY was calculated for patients ≤50 years, whereas it rose to €108,937/QALY for patients >50 years. The study was unique in that it incorporated the rate of crossovers in the AAD group to ablation, and the model was found to be most sensitive to the cost of ablation and readiness of offering crossovers.
Reynolds (2014)
The aforementioned studies examined cost-effectiveness of AF ablation by radiofrequency ablation. A recent paper was the first to analyse that of cryoballoon ablation, which utilises freezing rather than burning to isolate arrhythmogenic foci.38,42 Cryoballoon ablation was modelled from the UK perspective over a five-year time horizon as a second-line therapy compared with AADs in paroxysmal AF. They calculated an ICER of £21,957/QALY. The model was most sensitive to cost of follow-up care for recurrent AF and cost of ablation. Notably, the base-case ICER was comparable with that reported by the Rodgers/McKenna groups of radiofrequency ablation (£25,510/QALY).
Limitations, Future Directions
One-way sensitivity analyses of the above CEA studies show that the ICERs derived from their models are most sensitive to several input assumptions, which indicate areas requiring additional investigation. The three most commonly reported assumptions and input values were time horizon, the success rate of ablation and the QOL utility of restoring NSR. As such, for more accurate modeling, we must better determine the long-term effects that catheter ablation has on outcomes and costs, including maintenance of NSR, hospitalisations associated with recurrent AF to its relationship with heart failure, stroke and mortality. Ablation studies should also monitor patient QOL, instead of simply quantifying AF suppression rates and duration. Lastly, trends seen in AF ablation clinical trials such as high crossover rates should be accounted for when considering true definitions of first-line and second-line therapy.
As for future trends, our findings of ongoing cost escalation of AF ablation could cause the incremental cost of the procedure to rise to the point that ICERs may far exceed willingness-to-pay thresholds. Nevertheless, the field of electrophysiology is constantly evolving, and new research may improve cost effectiveness. For example, improved patient selection (of those with high likelihood of QOL improvement, not just those less likely to have AF recurrence), cost containment, and emerging approaches of ablation with higher success rates and improved durability of the ablation result could all substantially bend the cost curve. Judicious selection of procedure equipment could also lower expenditures, as ablation costs vary by material manufacturers: Reported prices of individual ablation device components (e.g. catheter, ultrasound, needles) reveal an impressive range for the cost of a single procedure from $6,637–$12,603USD (2013) based on cheapest and most expensive components respectively.43
New technologies could further cut costs by simplifying the procedure. Cryoballoon ablation was designed to obviate the need for a mapping system and creation of multiple ablative lesions, leading to shorter procedure times. On the other hand, standardisation of practice will be crucial, as many physicians perform radiofrequency with mapping at the same time as cryoablation, which would dramatically increase the cost.
Conclusions
In summary, assessing the value of AF ablation from a healthcare or societal perspective is challenging. ICER estimates are high, close to willingness-to-pay thresholds, and may have considerable uncertainty around them. However, the data show that ablation may be costeffective in the right patient. For first-line therapy, the procedure may not be cost-effective because of a moderate likelihood of treatment response. In the CEA studies that examined AF ablation as first-line therapy, the threshold values calculated for efficacy were closely tied to the assumptions of stroke risk/QOL improvements. They yielded ICERs <$50,000USD/QALY for procedural efficacy of 80 %–88 % and annual stroke risk of NSR ≤0.76 % or QOL improvement of -0.02 QALYs.30,36,37 But in symptomatic patients who fail AAD therapy, the studies indicate that AF ablation is generally cost-effective, particularly in younger patients with high symptom burden, as they are more likely to be alive longer and experience toxic side effects of pharmaceutical approaches.30 Advances both in cost-saving policies and novel technologies with greater success rates will continue to expand the pool of patients for whom ablation is a cost-effective solution.