Catheter-based ablation has been a well-established tool in the treatment of ventricular tachycardia (VT). However, the effectiveness of catheter ablation may be limited by its ability to access sites of arrhythmogenic tissue and achieve adequate lesion size in target areas without risking collateral damage. Antiarrhythmic surgery would be an effective alternative in such situations. Despite the potential usefulness of arrhythmia surgery, major drawbacks include invasiveness, prolonged hospital stays, higher morbidity and potential mortality.1 These limitations have been partially overcome with the development of minimally invasive surgical approaches and the integration of surgical and catheter-based approaches. We define hybrid ablation as an approach that combines surgical intervention for access and/or ablation, along with catheter mapping and ablation. In this article, we review hybrid techniques for VT ablation, discuss the role of hybrid ablation techniques in the contemporary management of VT and review the outcomes of hybrid approaches. We specifically review issues regarding patient selection, specific procedural considerations, safety and future directions.
A Historical Perspective of Interdisciplinary Collaboration
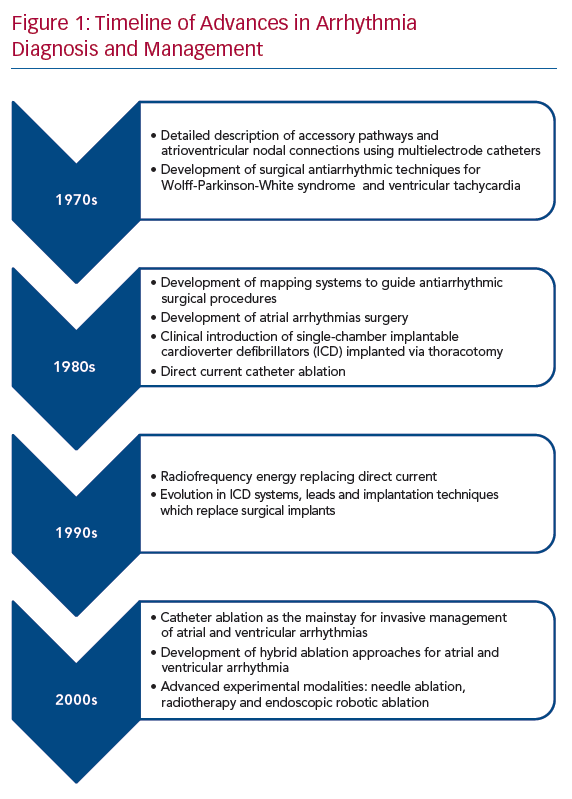
In the 1970s and 1980s, cardiac electrophysiological (EP) testing was extensively used for diagnosis and mapping of arrhythmias before or during cardiac surgery.2,3 With advancing EP knowledge and techniques, antiarrhythmic surgery was revolutionised (Figure 1). The foundation of this collaboration began with the Wolff-Parkinson-White (WPW) syndrome in which EP testing assisted in confirming the arrhythmia mechanism and determining the number and approximate location of accessory pathways.4,5 This expanded to include the encircling endocardial ventriculotomy introduced in 1978 for post-MI VT, the subendocardial resection procedure in 1979 for recurrent VT and the right ventricular disconnection procedures developed in the early 1980s for arrhythmogenic right VT.6–8 Furthermore, the introduction of steerable catheters in the 1980s and the development of 3D navigation systems in the last two decades allowed detailed EP mapping in a shorter time, which significantly improved preoperative planning for patients undergoing surgical approaches.
Patient Selection
Hybrid ablation combines the advantages of percutaneous endocardial and epicardial catheter-based procedures and those of arrhythmia surgery. In 1996, Sosa et al. initially described a subxiphoid percutaneous epicardial approach for epicardial mapping and ablation in patients with Chagas cardiomyopathy and associated VT secondary to epicardial substrates.9 The procedure has since been widely adopted in the management of ventricular arrhythmias in complex substrates. Epicardial approaches are often necessary for mapping/ablation of epicardial substrates, such as in patients with non-ischaemic cardiomyopathy including arrhythmogenic right ventricular cardiomyopathy, but also in order to provide an additional vantage point for creation of larger ablation lesions in patients with intramural substrate. However, safe percutaneous epicardial access may not be feasible in some patients. Some of the clinical scenarios where a hybrid approach may be necessary are listed below. These include situations where safe epicardial access may not be feasible and situations where power delivery to the area of interest would be insufficient.
Patients with extracardiac anatomical challenges, such as overlaying bowel loops, severe pectus deformity, rendering epicardial access prohibitively high risk.
Patients with extensive adhesions from previous open-heart surgery, pericarditis or epicardial procedures.10 Even with successful percutaneous access in patients with previous cardiac surgery, success rates are lower and the risk of complications can be significant.11 In addition to the limited catheter manipulation by adhesions, the adhesions themselves are sometimes vascular and catheter manipulation may lead to intrapericardial bleeding.
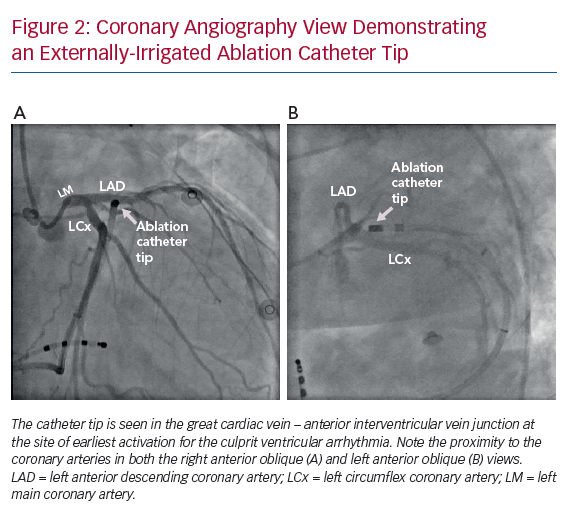
The myocardial tissue that needs to be targeted is in close proximity to critical structures, particularly the proximal coronary arteries making catheter ablation too high risk (Figure 2).
Need for epicardial mapping/ablation in patients with prior coronary artery bypass grafting (CABG). Even though percutaneous epicardial access in these patients is feasible, catheter manipulation and ablation carry a risk of graft disruption.12 Also, in patients with coronary artery disease, catheter manipulation during mapping and ablation can disrupt the bridging veins that traverse the pericardium to the myocardium as natural bypasses. Thus, the procedure in those patients carries a risk of infarction.12
Arrhythmogenic substrate or arrhythmia origin deep within the myocardium and below epicardial fat may not be amenable to catheter ablation via traditional percutaneous epicardial access. Direct visualisation is possible with surgical access and can permit epicardial fat dissection and surgical ‘unroofing’ of the target myocardium.
Inaccessible left ventricle (LV) due to mechanical aortic and mitral valves. While percutaneous transapical, transventricular septal or atrioventricular septal puncture can be performed, these approaches are limited to endocardial mapping and ablation. Given that such patients tend to have non-ischaemic substrate with perivalvular/epicardial substrate, an approach for epicardial mapping and ablation would be desirable.13
Surgical Approach
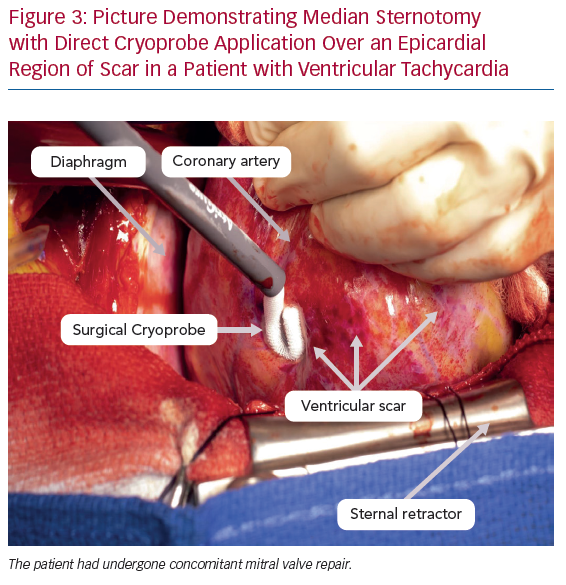
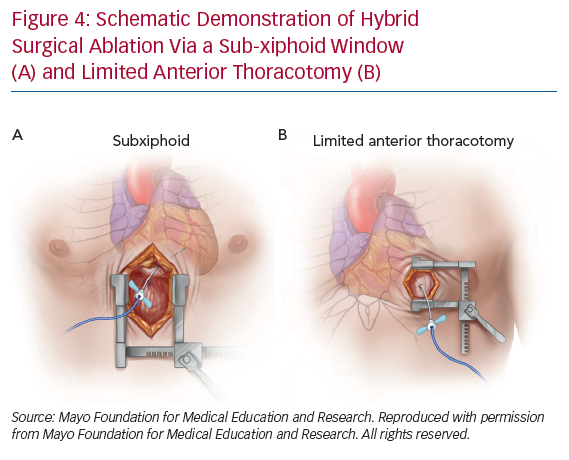
The surgical approach should be individualised and based on the likely origin/exit of the arrhythmia as determined by scar location on preprocedural imaging (typically MRI), non-invasive mapping, or prior invasive mapping. In particular, delineation of the arrhythmogenic substrate with preprocedural delayed-enhancement MRI has been associated with improved procedural and long-term outcomes in patients with non-ischaemic cardiomyopathy undergoing catheter ablation and this may also apply to hybrid procedures.14 While median sternotomy can provide wide access to the epicardial surface, this may be unnecessary and is associated with increased procedural time and morbidity (Figure 3). Therefore, in the absence of need for concomitant cardiac surgery, two main approaches are currently in use: subxiphoid window and limited anterior thoracotomy (Figure 4). Patient selection for each approach is critical due to the difference in LV epicardial exposure between the two.
Soejima et al. described a subxiphoid approach for VT mapping and ablation that provides access to the inferior and inferolateral LV.15 After dissecting down to the diaphragmatic pericardial surface, the pericardium is opened and under direct visualisation, lysis of any adhesions is performed with blunt dissection to fully expose the diaphragmatic and posterior epicardium. This approach is suitable for patients with predominately inferior or basal inferolateral scars.
Limited anterior thoracotomy provides access to the anterior, mid to apical anterolateral wall and the true apex. As such, it is suitable for individuals with previous scarring in the left anterior descending coronary artery territory. Typically, the procedure is performed under general anaesthesia. A limited left anterior incision is performed at the target intercostal space and extended through the subcutaneous tissue and fascia.16 The pericardium is then dissected off the LV laterally to maximally expose the area of interest.
A case report described a successful VT ablation using a transabdominal endoscopic approach using an incision through the central tendon of the diaphragm with concomitant use of an Impella haemodynamic support device (Abiomed) which was felt to be less invasive than performing a subxiphoid window.17 Another minimally invasive option that provides broad access to the epicardium includes a lateral thoracoscopic approach using one-sided three-port thoracoscopy.18,19
After the epicardium has been surgically exposed, the surgeon or electrophysiologist can proceed with direct catheter mapping and ablation with the guidance of a recording system and a 3D electroanatomic mapping system.
Depending on institutional practice and resources, such hybrid procedures can be performed either in the EP laboratory or in the operating room. This was demonstrated in a study of 14 patients who underwent hybrid surgical epicardial ablation with surgical access in the EP laboratory.16 However, whether this practice can be widely adopted depends on the availability of resources and expertise.
Electroanatomical Mapping
Surgical access allows epicardial mapping of ventricular arrhythmias during the hybrid surgical procedure. LV access could be obtained via the transseptal or retrograde aortic approach in cases of concomitant endocardial mapping. 3D electroanatomical mapping systems integrate anatomy with electrophysiology. These systems enable the display of catheter position in real time and permit geometrical reconstruction of the chamber of interest. Signals for voltage and activation mapping can be annotated simultaneously during baseline rhythm or tachycardia. Since their inception, 3D electroanatomical systems have facilitated the reconstruction of complex anatomical and EP considerations during procedures and increased safety, efficacy and efficiency of ablation compared with only using fluoroscopy.20 Of note, electroanatomic mapping and EP recording systems may not be readily available in the surgical suite. Portable systems are available but require knowledge and experience to set up and for troubleshooting.
Safety and Outcomes of Hybrid Ventricular Tachycardia Ablation
Several case reports and series have been published demonstrating the feasibility of the hybrid procedures.10,15,16,21 In 2004, Soejima et al. described their experience using the subxiphoid surgical window in six people with VT with prior cardiac surgery or failed percutaneous pericardial access.15 The study demonstrated the safety and feasibility of the approach. Access to the pericardium was successful in all patients. No complications were reported apart from transient chest pain consistent with pericarditis. After a follow-up period ranging from 106 to 675 days, two of the six patients had recurrent, though infrequent, VT.
In 2010, a multicentre study assessed the safety of epicardial VT ablation in 134 patients. Percutaneous subxiphoid approach failed in 10% of the cases (n=15). A surgical window for epicardial exposure was performed via a subxiphoid approach in 14 patients with no specific complications reported in this group.10 On follow-up, 95 of the 134 patients (71%) achieved freedom from recurrence after 23 (±21) months.
A recent study involved five patients who underwent hybrid ablation for recurrent sustained VT using combined endocardial and epicardial mapping and radiofrequency ablation in a hybrid operating room. Surgical approaches included anterolateral thoracotomy, one-sided three-port lateral thoracoscopy and sternotomy. After a mean follow-up of 18 months, three patients remained VT free with two of them using antiarrhythmics. One patient with recurrent VT required increasing amiodarone dose for arrhythmia control and one patient required a redo ablation 21 months after the initial procedure. There were no periprocedural complications.18
While these published experiences demonstrate the feasibility and safety of hybrid ablation in centres with experienced operators, no randomised studies have assessed whether this approach is superior to traditional catheter-based ablation in terms of long-term arrhythmia control. In a propensity-matched comparison of 38 patients who underwent hybrid epicardial ablation compared with patients who underwent percutaneous epicardial ablation, there was no significant difference in long-term outcomes.22
Endoscopic Robotic Ventricular Tachycardia Ablation
While robotically assisted endoscopic coronary artery bypass surgery was established as an alternative to the standard median sternotomy approach over the past two decades, its application in arrhythmia surgery had to await the evolution of technology. One of the most challenging scenarios electrophysiologists might face is the approach to arrhythmias arising from the LV summit. This region comprises the most superior portion of the LV epicardium, near the bifurcation of the left main coronary artery into the left anterior descending and left circumflex coronary artery. The complexity of the relationship between the LV summit and surrounding structures may limit the feasibility of safe ablation in this area. Access to the most basal aspect of the LV summit is also frequently limited by epicardial fat. As first described by Mulpuru et al., robotically assisted surgery could be used for these complex arrhythmias as they describe a successful case of resistant VT originating from the LV summit with a robotically assisted endoscopic mapping followed by a mini-thoracotomy and cryoablation.23 This was expanded upon by Aziz et al. with a totally endoscopic LV summit premature ventricular complex ablation performed using a duodecapolar catheter for mapping coupled with an externally irrigated radiofrequency ablation catheter.24 Such approaches allow for excellent visualisation of the coronary arteries in this sensitive area; furthermore, surgical dissection may permit the surgeon to mobilise adjacent arteries to allow safer delivery of ablative energy. This approach can offer an alternative option for targeting these challenging arrhythmias when standard approaches have failed. However, considerable operator skill and experience is required, especially if it is performed ‘off-pump’.
VT Ablation in the Setting of Left Ventricular Assist Device
People with advanced heart failure have a high incidence of ventricular arrhythmias. While left ventricular assist device (LVAD) implantation is associated with increased survival compared with conventional therapy in carefully selected patients, postoperative VT is common and may occur de novo in one-third of patients, which may be related to the new substrate associated with the apical core incisions but also due to pre-existing substrate.25 In LVAD patients, VT is associated with increased morbidity and mortality.26 Practical considerations regarding VT ablation in LVAD patients include crossing the aortic valve in the absence of complete valve opening due to loss of significant flow across the valve, or in some cases, over-sewing of valve leaflets.27 This, however, can be largely circumvented by accessing the ventricle using a transseptal approach.
While feasible, endocardial catheter ablation in patients with LVAD can be high risk. Therefore, mapping and ablation at the time of LVAD implantation surgery represent a novel approach to the management of this high-risk population. A large number of these patients have had previous endocardial mapping and this information can be used in conjunction with epicardial mapping intraoperatively. While mapping and ablation can typically be performed at the time of the surgery, often the sternum is not immediately closed after LVAD implantation.28 This period represents another opportunity for epicardial mapping and ablation in patients with suspected epicardial VT or substrate.29 Although adhesions limit percutaneous pericardial access after LVAD implantation, case reports have described ablation after LVAD implantation using lateral thoracotomy or subxiphoid approaches as has been described following non-LVAD cardiac surgery.30,31
Procedural Considerations for Hybrid Ablation
A thorough evaluation and multidisciplinary approach including cardiac electrophysiologists, cardiothoracic surgeons, anaesthesiologists, perfusionists and allied health staff are critical in the care of patients before hybrid ablation. These important procedural aspects should be considered and addressed.
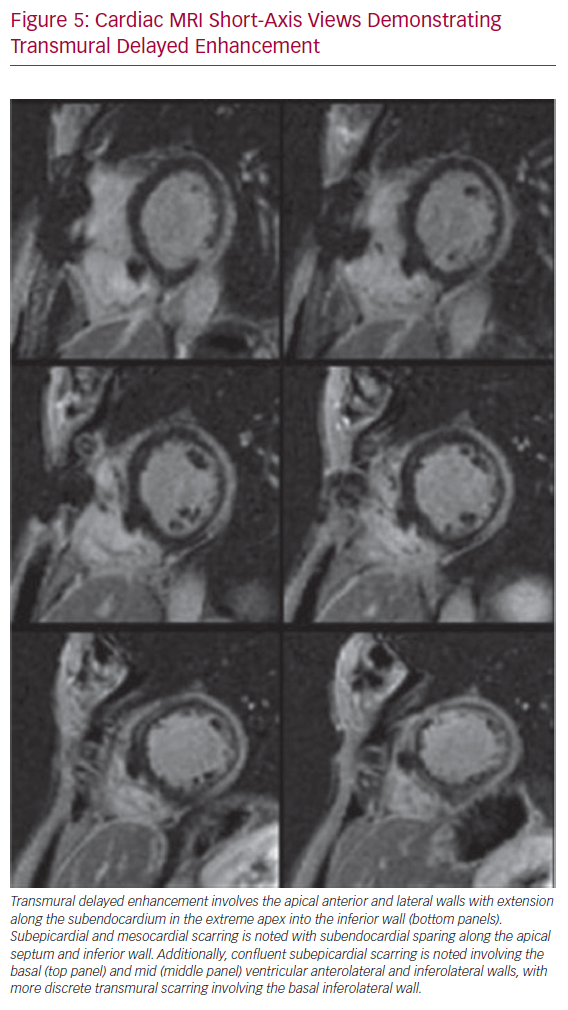
Preprocedural imaging is critical in order to define the distribution of the arrhythmogenic substrate (scar) and help determine the optimal hybrid approach. In most cases, cardiac MRI with delayed enhancement protocol will offer the most sensitive evaluation of the extent and location of scarring (Figure 5). Contrast cardiac CT scans can also be used.
Patients with a history of CABG should be evaluated with CT or invasive coronary angiography to determine the vessel course to assess the anatomic relationship to the selected surgical approach. CT may be effective in excluding large vessel stenosis/occlusion such as in graft vessels. However, its diagnostic value may be more limited for native vessels and invasive coronary angiography may be required.
In cases where an anterior thoracotomy is used, precordial ECG lead placement may be displaced from the standard position due to the incision line and this could affect ECG interpretation during mapping. The leads should be placed as close to the normal position as possible.With the limited anterior thoracotomy approach, single lung ventilation may be needed to allow for the appropriate exposure. Therefore, patients with severe respiratory lung disease may not be suitable candidates.
With severe pericardial adhesions, the surgeon may need to re-enter the thorax at a different intercostal space to extend exposure.16
In cases using minimally invasive access, such as robotic access, air accumulation in the pericardial space may increase the defibrillation threshold significantly. As such, one should be ready to deliver implantable cardioverter defibrillators (ICD) shocks, if available, or to evacuate air promptly to permit external defibrillation.32
The metal retractors used for surgical access can interfere with the electroanatomic mapping systems and consequently prohibit mapping in certain areas of the heart.
Ablation tools commonly used in the surgical setting use either cryoablation energy or radiofrequency. Cryothermy uses either Argon gas (CryoFlex, Medtronic) or nitrous oxide (cryoICE, AtriCure) to achieve rapid cooling temperature and deliver deep lesions. Flexible cryoprobes have the advantage of delivering tailored lesions over a wider area compared with radiofrequency. Some radiofrequency ablation devices, such as Cardioblate iRF (Medtronic) and Isolator (AtriCure) allow for mapping as well as ablation at the same time, which is not feasible with large cryoprobes.
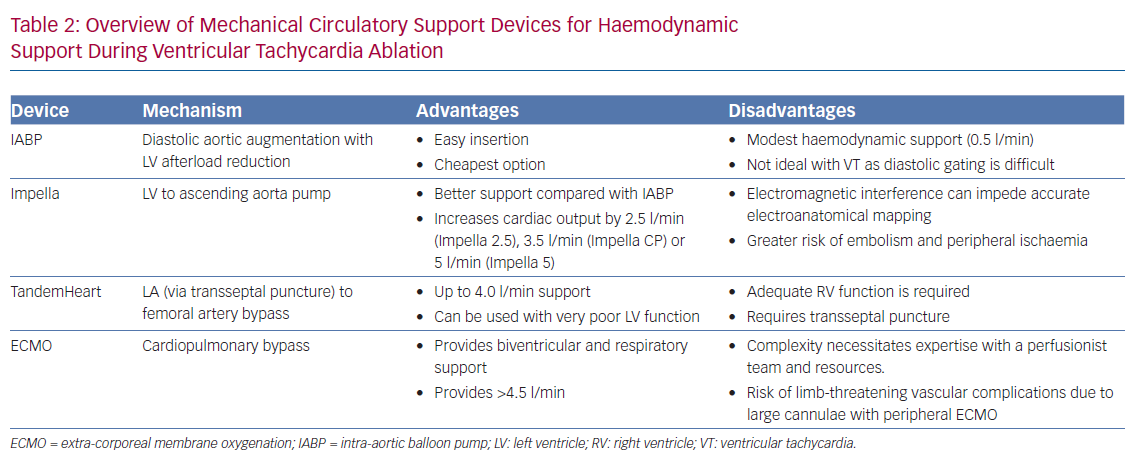
Haemodynamic decompensation from prolonged procedural time or during activation mapping of VT is a major limitation. While vasopressor and inotropic support are often used, these are frequently insufficient.33 Therefore, preprocedural risk stratification to assess for the need of potential mechanical circulatory support (MCS) is essential. Patients with advanced age, marked left ventricular dysfunction and comorbidities such as chronic obstructive pulmonary disease and diabetes are at particular risk for haemodynamic decompensation.34 MCS can be instituted at the beginning of the procedure, especially when activation mapping of unstable VTs is considered necessary. Alternatively, MCS may be established ad hoc, though it should be noted that the outcomes of urgent or emergent MCS for haemodynamic compromise during VT ablation procedures are poor. Short-term MCS options include intra-aortic balloon pump, Impella, TandemHeart (TandemLife) and extracorporeal membrane oxygenation (Table 2).35–37
Post-operative pain is a major issue and may be related to the route of access – such as sternotomy, intercostal access or rib retraction – tissue injury from ablation with associated inflammation and surgical drain sites. Inadequate management of post-operative pain prolongs the rehabilitation period and worsens patient-reported outcomes.38 As such, post-operative pain assessment and appropriate management are crucial.
Management includes multimodal analgesia such as non-steroidal anti-inflammatory drugs (NSAIDs), acetaminophen, as well as opioid and non-opioid analgesics; occasionally, regional anaesthesia may be used for refractory and prolonged pain.39 Pericarditis is also common following epicardial ablation and measures aimed at reducing pericardial inflammation should be instituted; these predominantly include NSAIDs and colchicine. In certain circumstances, intrapericardial or systemic steroid use and intrapericardial lidocaine may be used.40–42
Emerging Technologies in Ventricular Tachycardia Ablation
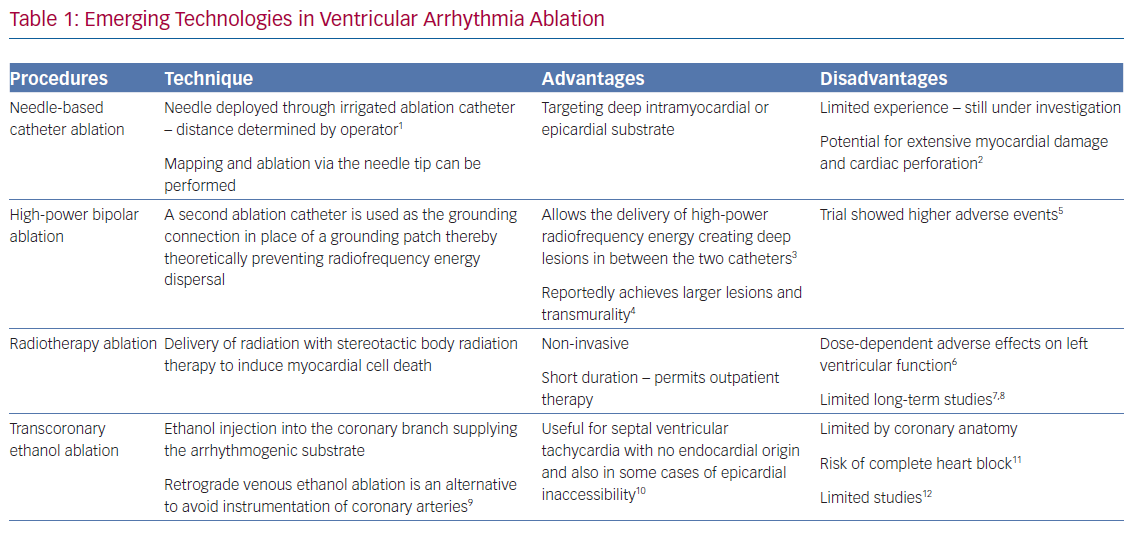
Though hybrid surgical ablation has provided another tool for the treatment of ventricular arrhythmias, emerging techniques may reduce the reliance on this approach. These remain off label and are mainly relegated to use in tertiary referral centres. Such techniques include needle-based catheter ablation, radiotherapy ablation, bipolar ablation and transcoronary or retrograde venous ethanol ablation (Table 1).43–53
Conclusion
The evolution of VT ablation techniques is associated with expanding indications. The choice should be guided primarily by the clinical scenario. Hybrid surgical ablation may be viewed as a form of synergism that combines the advantages of EP and surgery. There is now a significant body of evidence suggesting the safety and feasibility of hybrid surgical ablation of VT. Appropriate patient selection is key. Therefore, providers should be fully aware of the indications and caveats associated with this technique.
Clinical Perspective
- An increasing body of evidence suggests that hybrid surgical ablation is a safe, effective and feasible technique.
- Hybrid ablation should be considered in patients with pericardial adhesions, deep myocardial substrate, proximity to critical structures, inaccessible LV and extra-cardiac anatomic challenges.
- A multidisciplinary approach including cardiac electrophysiologists, cardiothoracic surgeons, anaesthesiologists, perfusionists and allied health staff is critical in the care of these patients.